Conventional wisdom says “less is more”. Just like the old-fashioned notion of needing to toughen your nipples for breastfeeding that has been de-bunked, you don’t need to do anything to help your body get ready for labor. In fact, you can cause more problems by trying to get labor going than if you just wait for labor to start on its own.
By trying to self-induce labor, you may start intense cramping that feels like labor, but isn't. Intense cramping can disrupt your sleep, leaving you too exhausted for the real thing. The most productive contractions, the ones that make cervical change, aren't the ones we force on ourselves, but the ones that evolve on their own.
When do most women give birth?
Before 40 weeks: 40% (+/- 10%).
After 40 weeks: 60% (+/- 10%).
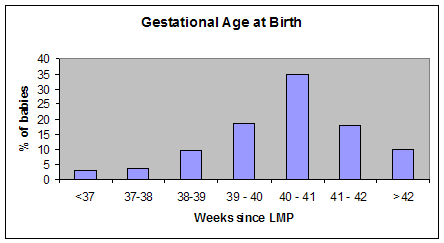
http://www.transitiontoparenthood.com/ttp/birthed/duedatespaper.htm Please see Janelle Durham’s excellent 2002 paper on Calculating Due Dates and the Impact of Mistaken Estimates of Gestational Age. She created the graphic above.
The most accurate way to calculate your due date is to count back 3 months from the first day of the last menses, then add 15 days for for first time mothers (or 10 days for multiparas). http://www.ncbi.nlm.nih.gov/pubmed/2342739
How Labor Starts On Its Own
Complex hormonal communication between your body and your baby signal the start of labor. That chemical communication starts weeks before labor and intensifies in the days and hours before active labor begins. Here’s what happens:
1. The baby starts everything! When your baby is ready to be born, he or she will secrete a hormone called CRH (cortico-releasing hormone) which sends a chemical signal to your placenta.
|
2. When your placenta receives the chemical signal from baby, it will release estrogen and cortisol, two hormones that will help your baby’s lung’s mature.
|
3. Now that the placenta is producing more estrogen, that chemical signal tells your uterus to create more oxytocin receptor sites within the uterine muscle which means you’ll likely have more Braxton Hicks contractions.
|
4. The increased estrogen production by your placenta also promotes the release of prostaglandins by the amniotic membranes. Prostaglandin is a hormone that produces enzymes that will digest the collagen in the cervix, turning it to water, causing the cervix to soften and become thin.
|
5. In late pregnancy, the placental membranes normally become increasingly fragile, porous and permeable, which means larger molecules from mother’s bloodstream like iron and maternal antibodies can finally cross the placenta, which means baby will gain important immunities from you and about six months worth of iron.
|
6. Your ovaries will secrete relaxin, a helpful hormone that relaxes all of your ligaments and cartilage during pregnancy, making the your pelvic joints wider and more mobile. That’s especially important in late pregnancy because your baby is descending and engaging in your pelvis, trying to find the best, most efficient position for birth.
|
| 7. The placenta begins making connexin, a hormone that helps the uterus contract in an efficient, coordinated way. These hormonal reactions will likely cause you to have a restless backache before you have synchronized, progressing contractions which eventually cause your cervix to open. |
All of these chemical reactions and coordinated release of hormones take time. Your patience is well worth it: You’ll have the best chances at the healthiest baby and the smoothest labor if you wait for labor to begin on its own.
Simkin, Penny, Whalley, Janet, Keppler, Ann, Durham, Janelle, Bolding, April. Pregnancy, Childbirth and the Newborn. New York, Meadowbrook Press, 2010
http://www.sarahbuckley.com/downloads/Ecstatic-Birth.pdf
http://www.nature.com/scientificamerican/journal/v13/n2/full/scientificamerican0503-80sp.html
Risks of self-inducing labor and why it may be better to leave well enough alone.
Castor oil induction – Nausea, vomiting and diarrhea leads to maternal dehydration and ineffective contractions
Cramping related to castor oil may feel like labor but may only produce ineffective contractions that don’t change the cervix and disrupts rest and sleep, leaving mother exhausted and ill. The stress on the mother’s body may also stress the baby, causing an increased likelihood of passing meconium. Meconium in the amniotic fluid can increase a baby’s likelihood of developing respiratory infection and the need for more medical intervention at the time of birth. http://www.ncbi.nlm.nih.gov/pubmed/11406076
Membrane stripping– Discomfort. More bleeding. More irregular, unproductive contractions. (Longer latent labor phase with inability to rest.) Perhaps more prelabor rupture of membranes due to unproductive contractions. http://www2.cochrane.org/reviews/en/ab000451.html
Nipple stimulation – Too much nipple stimulation can result in raw, irritated nipples that may increase pain during initial breastfeeding.
What is the risk of still birth after 40 weeks?
Risk of Still Birth By Week of Pregnancy
|
Week of
Pregnancy
|
Rate of
Still Birth
|
Likelihood this
will not happen
|
% Change
from 40 weeks
|
| 36 |
.39: 1000 |
99.961% |
- 55% |
| 37 |
.30: 1000 |
99.970% |
- 66% |
| 38 |
.52: 1000 |
99.948% |
- 40% |
| 39 |
.49: 1000 |
99.951% |
- 44% |
| 40 |
.87: 1000 |
99.913% |
0% |
| 41 |
1.27: 1000 |
99.873% |
+ 46% |
| 42 |
1.55: 1000 |
99.845% |
+ 78% |
| 43 |
2.13: 1000 |
99.787% |
+ 149% |
(BMJ, 2000 Feb 12)
Look at the table above. What your care provider might tell you: “Remaining pregnant beyond 42 weeks more than doubles your risk of still birth”. While the relative risk of still birth has more than doubled between 40 and 43 weeks gestation, the absolute rate of still birth remains small, rare in fact.
Are there benefits to inducing women’s labors at 41 – 42 completed weeks of pregnancy?
The 2006 Cochrane Library review of induction of labor for improving birth outcomes for women at or beyond term seems to show some benefits of inducing labor between 41 – 42 completed weeks of pregnancy. There were fewer still births in labors that were induced at 41 completed weeks of pregnancy. However, since the absolute risk is extremely small, women should be counseled on the benefits of induction for a prolonged pregnancy vs the risks of induction. http://www2.cochrane.org/reviews/en/ab004945.html
What are the risks of induction?
• Changes in fetal heart rate (non-reassuring fetal heart tones)
• Increased risk of infection in the woman and baby
• Umbilical cord problems
• Overstimulation of the uterus
• Uterine rupture
Inductions, in particular for first-time, mothers result in an increase risk of cesarean birth. Women use more pain medication with induced labors vs spontaneous labors. http://www.acog.org/publications/patient_education/bp154.cfm
http://journals.lww.com/greenjournal/Abstract/2000/06000/Elective_Induction_of_Labor_as_a_Risk_Factor_for.26.aspx
When to Use Medical Interventions:
| YES |
Choose medical interventions when the benefits of the intervention clearly outweigh the risks. |
| NO |
Any intervention used for convenience can result in HIGHER complication rates for mother and baby. |
| MAYBE |
When there is a gray area (benefits and risks may be similar or unclear), consider:
- Is mother okay now? Is baby okay now? Consider waiting a little longer before acting.
- Is this a routine procedure that you offer everyone or is there something unique about my situation? If routine, consider waiting a little longer.
- Who benefits from the intervention now? Mother, baby, care provider? If only the care provider benefits, consider waiting a little longer.
|